Faith & Family
Healthy meals to cook with your grandkids
Cooking with grandkids can be a fun, rewarding and memorable experience. Learn how to make the most of your moments in the kitchen together.
Read article

Showing 1–48 of 48
-
 Faith & FamilyRead article
Faith & FamilyRead articleHealthy meals to cook with your grandkids
Cooking with grandkids can be a fun, rewarding and memorable experience. Learn how to make the most of your moments in the kitchen together. -
 Faith & FamilyRead article
Faith & FamilyRead articleThinking about forming a Bible study? Start here.
Trying to start a Bible study? It’s easy to get lost in the logistics and feel overwhelmed. -
 Faith & FamilyRead article
Faith & FamilyRead articleRenew your strength in the Lord
Let the peace of Christ rule in your hearts ... and be thankful.
– Colossians 3:15 (NIV)
-
 Faith & FamilyRead article
Faith & FamilyRead articleQuestions for grandparents to ask their grandchildren
When talking to your grandkids, help them express a range of emotions — happy, sad, frustrated or amused. And be open to listening to any topic. -
 Faith & FamilyRead article
Faith & FamilyRead articleWhat staff members need to know about family caregivers
Family members and friends who are responsible for looking after and helping their loved ones are an extremely valuable part of the care team for Good Samaritan Society residents living in long-term care. -
 Faith & FamilyRead article
Faith & FamilyRead articleHow caregivers and older adults can cope with holiday stress
Many caregivers and older adults struggle with stress during the holidays. Find strategies for coping with the stress of the season here. -
 Faith & FamilyRead article
Faith & FamilyRead articleThoughtful gift ideas for seniors
Buying Christmas gifts for seniors or grandparents can be a thoughtful and rewarding experience. But it can also be difficult! When buying gifts for seniors or grandparents in your life, think about your loved one’s hobbies, interests and preferences. -
 Faith & FamilyRead article
Faith & FamilyRead article5 Ways to be an active listener
Research shows that social isolation takes a toll on our mental health, well-being and quality of life, especially as we age. Thanks to advancements in technology, we are able to stay connected with loved ones through to texting, social media and video-chats. While that type of connection is important, in-person connections are still vital for older adults. -
 Faith & FamilyRead article
Faith & FamilyRead articleThe importance of advance care planning and directives
Advance directives are state-specific legal documents for communicating end-of-life and care wishes. Learn why it's important to create one and how to do so. -
 Faith & FamilyRead article
Faith & FamilyRead articleHow to cope with the holiday blues
Everyone has a unique mix of life experiences, cultures, traditions and memories surrounding the holidays. Take time to acknowledge and value your perspective and the perspectives of others. -
 Faith & FamilyRead article
Faith & FamilyRead articleAlzheimer's and the holidays
Although the holidays are a time for rejoicing, this time of year can be stressful for those with Alzheimer's. Read how to make the holidays more comfortable for people with memory loss. -
 Faith & FamilyRead article
Faith & FamilyRead articleWhat feels like the end is often the beginning
On a Monday back in March of 2020, I was clocking back in after lunch at Cedar Lake Village when I noticed a sign on the wall that caught my attention. -
 Faith & FamilyRead article
Faith & FamilyRead articleCoping with grief
When someone you love dies, the grief can feel overwhelming. Take steps toward healing while remembering and honoring your loved one with these five strategies. -
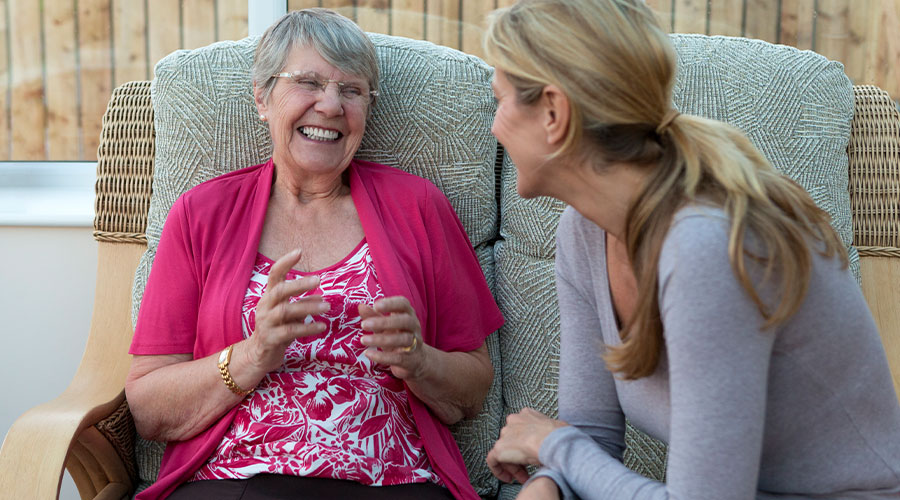 Faith & FamilyRead article
Faith & FamilyRead articleHow do you talk to someone who has Alzheimer’s?
No matter how deeply we care about friends or family, Alzheimer’s disease or dementia can make us uncomfortable — especially when we don’t fully understand it. -
 Faith & FamilyRead article
Faith & FamilyRead article10 ways to boost your mood
We all face times in our lives when we feel overwhelmed by worry, uncertainty, loss or loneliness. To cope with life’s ups and downs, use these 10 tips to boost your mood and stay positive. -
 Faith & FamilyRead article
Faith & FamilyRead articleGod’s love endures forever
Researchers who study such things say it usually takes at least five times before you begin to remember the information. Of course, the longer the list or sentence, the more times it can take for even those with great abilities to commit it to memory. -
 Faith & FamilyRead article
Faith & FamilyRead articleMissionaries wherever we are
Scripture teaches us that we can be a witness to Christ no matter where we are. -
 Faith & FamilyRead article
Faith & FamilyRead articleTips for talking to your parents about getting in-home medical care
Use the following conversation starters to help you talk about how home care could benefit your mom or dad — and you. -
 Faith & FamilyRead article
Faith & FamilyRead articleThe Good Samaritan - none other than Jesus himself
March 13 marks Good Samaritan Day – a fitting time for the Good Samaritan Society to celebrate our namesake. -
 Faith & FamilyRead article
Faith & FamilyRead articleHow to start preserving your family history
Our family narrative tells the stories of who we are. When we look back on memories from birthday parties, graduations, weddings and other special moments, we are provided with a greater sense of self. -
 Faith & FamilyRead article
Faith & FamilyRead articleHow to cope when your spouse is facing health issues
Cathy Rosch’s relationship with her husband, George, shifted when he suffered a traumatic brain injury and she became his caregiver. -
 Faith & FamilyRead article
Faith & FamilyRead articleA Christmas devotional
“And the Word became flesh and lived among us.” John 1:14 (NRSV) -
 Faith & FamilyRead article
Faith & FamilyRead articleDo I need advance care planning?
Not sure if you need to outline your healthcare preferences and end-of-life wishes? -
 Faith & FamilyRead article
Faith & FamilyRead articleHow do you know if you’re a caregiver?
You check the mail for Mom since you're already at the post office. -
 Faith & FamilyRead article
Faith & FamilyRead articleGrieving the loss of a loved one over the holidays
After losing a loved one, the Christmas season can be a challenging time to grieve and heal. You may experience a wide array of emotions that become especially difficult to process amid festive holiday décor, gatherings and activities. -
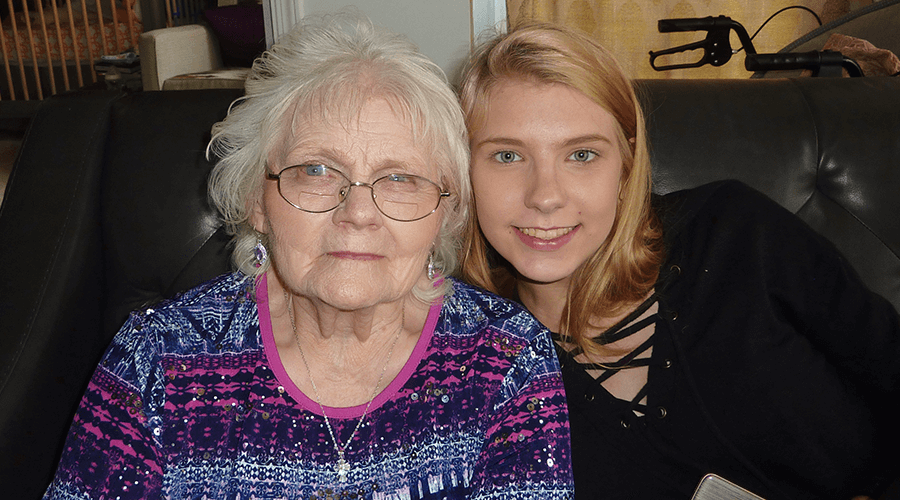 Faith & FamilyRead article
Faith & FamilyRead articleChallenges stack up for sandwich generation caregivers
With the population of Americans over 65 growing steadily, the number of adults who care for an aging parent while also caring for their children is increasing, too. -
 Faith & FamilyRead article
Faith & FamilyRead articleSigns your parent needs help at home
Read about potential signs that your loved one needs assistance at home as well as five things you can do to help. -
 Faith & FamilyRead article
Faith & FamilyRead articleLong-distance caregiving brings unique challenges
Caregiving from a distance can be complicated. Whether the task is big or small, helping from a distance adds layers of complexity to any task. But you're not alone. -
 Faith & FamilyRead article
Faith & FamilyRead articleThe Ultimate Gift
In the midst of Christmas busyness this year, take a moment to remember God’s Ultimate Gift to you: his one and only Son. -
 Faith & FamilyRead article
Faith & FamilyRead articleFear is knocking — do not open the door
Have you ever had someone knock on your front door and when you peek through your peephole, it's someone you don’t want to see? You hope they didn't hear you coming to the door or the kids talking or maybe the dog barking. You wait to see if they will go away, but they knock even harder. So you open the door and let them in. They settle in and make themselves at home. You wish they would leave, but they won't go — after all, you let them in. -
 Faith & FamilyRead article
Faith & FamilyRead articleMother’s Day gift ideas
This year might still look a little different, but it’s important to take time to celebrate the women who make your life better. -
 Faith & FamilyRead article
Faith & FamilyRead articleThe power in acceptance
When you’re dealing with challenging circumstances, there’s a power and freedom that come with acceptance. We asked the Rev. Greg Wilcox, senior pastor at the Good Samaritan Society, to share his insights. -
 Faith & FamilyRead article
Faith & FamilyRead articleAmid COVID concerns, plan ahead and consult family when contemplating a change of address
There are always going to be at least two parts to the decision to move. -
 Faith & FamilyRead article
Faith & FamilyRead articleAre you ready to ‘fare well’?
Too often, if a health crisis occurs, we do not have a power of attorney, an advanced directive, or the reassurance of prior conversations with our family about our wishes in case of illness or death. -
 Faith & FamilyRead article
Faith & FamilyRead articlePreventing elderspeak when addressing older adults
While many caregivers feel like speaking in a cheerful, simple way or using terms of endearment shows they care, many older adults are less than receptive to this manner of speech. -
 Faith & FamilyWays to grow your faith
Faith & FamilyWays to grow your faith4 ways to grow in your faith
As people of faith, it’s important to nurture our spiritual side. But many of us tend to get comfortable doing the same type of faith practice year after year. -
 Faith & FamilyRead article
Faith & FamilyRead articleSimple ways to pay it forward
Hebrews 10:24 (NIV) encourages us to be an example for others to follow. -
 Faith & FamilyRead article
Faith & FamilyRead article7 encouraging Bible verses
Rev. Dr. Julie Berndt of the Good Samaritan Society and Sanford Health shares Scripture verses to bolster your spiritual health if you are living with a long-term illness or caring for someone who is. -
 Faith & FamilyRead article
Faith & FamilyRead articleA lesson in grace
I have 8-year-old twin boys, Jeremiah and Joshua. They look completely different from each other, and yes, they act completely different, too. -
 Faith & FamilyRead article
Faith & FamilyRead articleTips for building a prayer
Have you ever been asked to lead a prayer, out loud, in public? Were you prepared? -
 Faith & FamilyRead article
Faith & FamilyRead articleBreak the silence around domestic violence
Any incident of domestic violence is unacceptable. -
 Faith & FamilyRead article
Faith & FamilyRead article6 fun ideas to bring children, older adults together
Want to help your children interact with older adults? Want a better relationship with your grandchildren? Consider these ideas as you brainstorm fun activities. -
 Faith & FamilyRead article
Faith & FamilyRead articleThe best states for family caregivers
Caring.com says 10 states are doing the best job of easing the financial burden on caregivers of older adults and providing mental, emotional and physical support. -
 Faith & FamilyRead article
Faith & FamilyRead articleWhat about prayer?
These days we schedule almost everything. There is a system or methodology for almost every aspect of our lives. -
![Death does not have the final word. God does. [slideshow] Death does not have the final word. God does. [slideshow]](/-/media/project/good-sam/resources/items/2255_fam_sm-940px.jpg?h=140&iar=0&w=264&hash=765C31ECA458204C26F82619A9EC8012) Faith & FamilyRead article
Faith & FamilyRead articleDeath does not have the final word. God does. [slideshow]
A life well lived includes dying well; that is, having spiritual, emotional, physical and social needs met at the time of a loved one's death. -
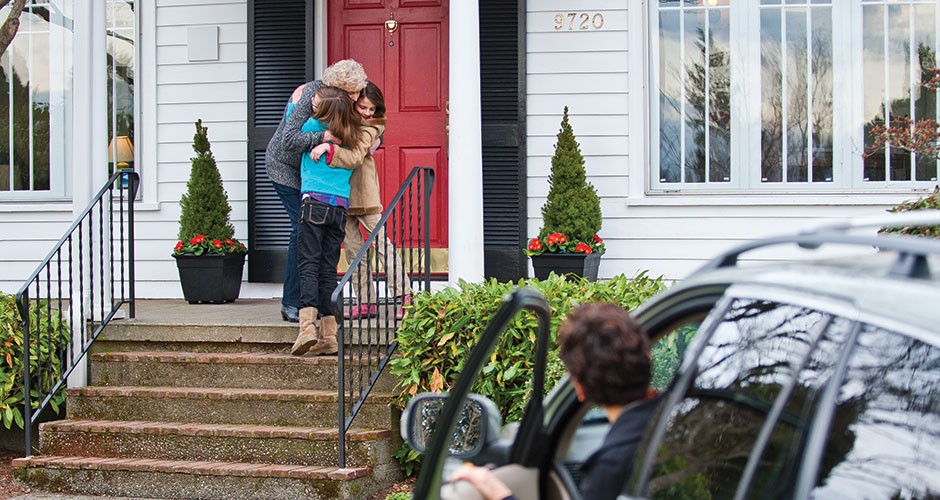 Faith & FamilyRead article
Faith & FamilyRead article7 ways to connect with your grandkids
You can be so much more to your grandchildren than just candy givers, toy buyers and kid spoilers. -
 Faith & FamilyRead article
Faith & FamilyRead article26 questions to spark great conversations
Whether it’s strangers at the table, family members at a reunion or new co-workers in the hallway, we all have people we struggle to make conversation with. -
 Faith & FamilyRead article
Faith & FamilyRead articleLet prayer outshine worry
In the book of Philippians, Paul is writing to people in a church in Philippi. The Philippians are struggling, and Paul himself is in prison.
Find a Good Samaritan Society location
Connect with Us
Sign up for the Good Samaritan Society's newsletter to learn about our mission and how we're making a difference. Stay up-to-date on health information, events, services, and more.
